- 01865317483, 07856131431
- help@gbclinics.co.uk
Understanding MSK Pain:
A Clinician’s Perspective on Diagnosis and Recovery at GB Clinics
Musculoskeletal pain—what we in the clinic call MSK pain—is something I’ve come to know not just through textbooks or scan results, but through people. Through stories. It’s the mother who can no longer kneel to play with her child, the runner who hesitates before every stride, the office worker who dreads the ache that creeps in after a few hours at the desk.
It doesn’t always start dramatically. Sometimes it begins with a bit of stiffness in the shoulder, or a dull pull in the lower back after a weekend spent gardening. People often tell me, “It’s nothing, just a niggle.” But over time, that niggle becomes a pattern. A limp. A hesitation. A subtle change in the way someone moves, rests, or even thinks about their body.
At GB Clinics, we meet people every day who have been quietly adjusting their lives around pain. What I always say is this: just because it’s common doesn’t mean it’s normal. MSK pain deserves attention. It deserves proper diagnosis. And in most cases, it deserves a plan—not guesswork.
Let’s talk about what that looks like.
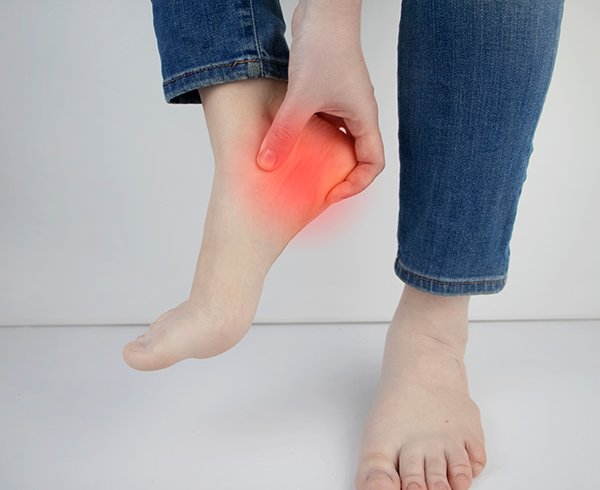
What Is MSK Pain, Really?
When we say “musculoskeletal pain,” we’re referring to discomfort that arises from the structures that support movement—muscles, bones, joints, tendons, ligaments, and sometimes even the nerves that run alongside them. It’s a broad term, but it’s not vague. It’s just that the human body is an interconnected system, and pain rarely exists in isolation.
Some patients describe it as a sharp jolt when they move a certain way. Others say it’s a dull, constant pressure that follows them throughout the day. Sometimes it’s felt in one place. Sometimes it radiates. And occasionally, it’s hard to describe at all.
But here’s the important part: MSK pain is never just about physical sensation. It touches everything—mobility, sleep, mood, relationships, even the confidence to plan a weekend walk or say yes to an activity.
And too often, it’s overlooked.
"It’s Just Ageing"—A Common Myth
Many people come to us saying, “I guess it’s just age,” as though discomfort is the price of getting older. While age-related changes in our bodies are real, they are not a reason to accept pain as inevitable.
More often, MSK pain has causes that are specific, identifiable, and treatable. Let’s go through a few of the most common ones we see in clinic.
Arthritis
Arthritis is often feared, but misunderstood. The most common type—osteoarthritis—happens when the cartilage that cushions your joints wears down over time. Without that protection, bones rub against each other, leading to pain, swelling, and stiffness. But it’s not just wear and tear—it’s about inflammation, joint mechanics, and sometimes activity choices too.
Then there’s rheumatoid arthritis, which is an autoimmune condition. It causes the immune system to mistakenly attack the joints, leading to more widespread symptoms including fatigue.
The key message? Early management matters. Arthritis can be managed—not ignored. And with the right care, many people live active, pain-limited lives.
Past or Recent Injuries
Some people come in with fresh injuries—a fall, a strained muscle, a twisted knee. Others come in years after an injury they thought had healed. Sometimes the pain is from the original problem. Sometimes it’s from compensating for it over time.
What I tell patients is this: even if something feels “minor,” if it lingers, it deserves a proper look. Old injuries that weren’t properly treated can lead to long-term movement changes, weakness, or instability.
Repetitive Strain
Our daily habits shape our bodies more than we realise. Lifting a child the same way every day. Typing at a laptop for hours. Driving long distances. Sleeping in the same curled-up position.
These movements aren’t bad in themselves, but done repeatedly—and sometimes without enough balance or rest—they create what we call micro-trauma. Over time, this can lead to things like tendinopathy, bursitis, or muscle fatigue.
It’s the kind of pain that builds slowly and often goes undiagnosed for too long.
Posture and Alignment
This is a big one. Most people today are sitting more than ever before—working from home, commuting, or simply living in a digital world. Poor posture places strain on joints, muscles, and supporting structures.
When alignment is off, the body starts to compensate. Some muscles tighten, others weaken. Before long, you’ve developed patterns that lead to discomfort—and sometimes even persistent pain.
But with assessment, guidance, and the right kind of movement, these patterns can be retrained.
Why Diagnosis Matters More Than Guesswork
I can’t count the number of times I’ve met people who’ve been given painkillers, told to “rest,” or handed a generic list of exercises printed from the internet.
That’s not treatment. That’s a holding pattern.
The first step toward meaningful recovery is accurate diagnosis. And that starts with listening.
- At GB Clinics, we take the time to really hear your story:
- When did the pain begin?
- What makes it better—or worse?
- What do you do during the day?
- How do you sleep, sit, and walk?
- Every detail gives us clues.
- And when it’s needed, we turn to one of the most helpful tools in modern MSK care: diagnostic ultrasound.
Why We Use Ultrasound at GB Clinics
When people hear “ultrasound,” they often think of pregnancy scans. But in MSK medicine, it’s a non-invasive, real-time window into the body’s moving parts.
Unlike X-rays or MRIs, which are static, ultrasound lets us observe joints and soft tissues as they function. That’s incredibly valuable—because many MSK issues only show up during movement.
- We use ultrasound to:
- Detect swelling, inflammation, or fluid
- Visualise tendon or ligament damage
- Identify impingement or structural abnormalities
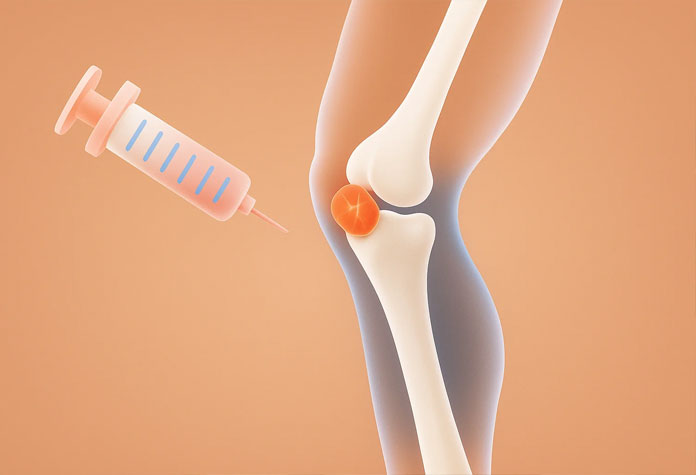
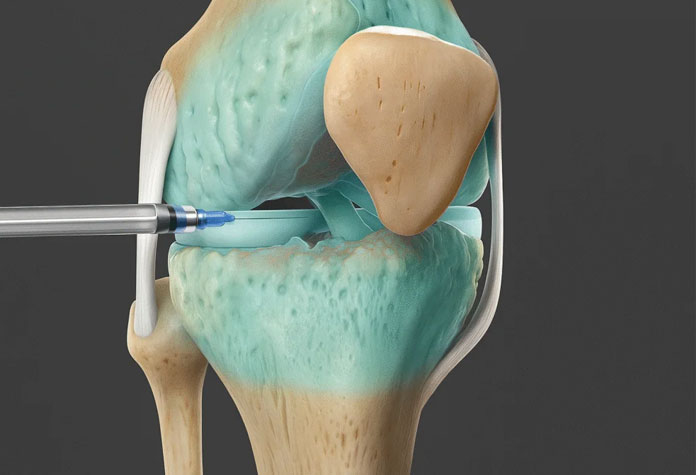
- Guide injections with pinpoint accuracy
- What’s more, all ultrasounds at GB Clinics are performed by clinicians trained specifically in MSK medicine. So your scan isn’t just done—it’s interpreted, explained, and used to guide a plan right then and there.
What the GB Clinics Journey Looks Like
Our approach isn’t rushed, and it isn’t fragmented. We believe your care should flow. Here’s what your journey might look like with us:
🩺 Step 1: Consultation
We begin with a conversation—about your pain, your life, your goals. We don’t see you as a diagnosis, but as a person with a story.
🖥 Step 2: Real-Time Imaging
If needed, we perform an ultrasound during your visit. You’ll see the images, and we’ll explain exactly what’s happening.
🧭 Step 3: A Plan That Fits
- Once we understand the root cause, we create a care plan that works for your body and your schedule. That might include :
- Physiotherapy to restore strength and mobility
- Massage therapy to ease tension and improve circulation
- Podiatry to assess foot mechanics and posture
- Shockwave therapy for stubborn soft tissue problems
- Injections, where appropriate, guided with precision
🧘♀️ Step 4: Personalised Movement
Recovery isn’t just about rest—it’s about smart, safe movement. Our physiotherapists work alongside consultants to build a plan that’s responsive, not rigid. Your progress is reviewed and adjusted as needed.
🔄 Step 5: Maintenance and Prevention
Once you’re better, we help you stay that way. That may include ergonomic advice, postural corrections, strengthening routines, and simple daily changes.
Pain-free is good. Staying pain-free is better.
Why Patients Choose GB Clinics
- Here’s what many of our patients say sets us apart:
- Consultant-led care with years of combined experience
- On-site ultrasound scans and same-day appointments
- No unnecessary waiting or referrals
- Treatments and therapies under one roof
- A team that communicates—and truly cares
- A calm, welcoming environment
- We’re proud of the clinical expertise we offer. But what we’re most proud of? Our time with you is yours. We don’t rush. We explain. We listen.
When Should You Seek Help?
- If you’re unsure whether it’s time, consider these signs:
- Pain lasting more than two weeks
- Recurrent pain in the same area
- Discomfort interfering with sleep, walking, or work
- Reduced strength or flexibility
- Failure to improve with rest or home exercises
- You don’t need to be in crisis to benefit from proper MSK care. In fact, earlier attention often means faster, fuller recovery.
Living Well, Again
We’ve seen people go from avoiding stairs to living a normal life again. From hesitating before bending to picking up their grandchildren with ease. The goal isn’t just relief—it’s restoration. Confidence. Freedom in movement.
MSK pain might be part of your story now—but it doesn’t have to be the whole story.
Ready to Move Better?
If you’re tired of guessing, hoping, or putting it off, maybe now’s the time to find out what’s really going on—and what you can do about it.

Book your visit at GB Clinics Oxford.
We’ll meet you where you are. And help you get where you’d like to be.
