- 01865317483, 07856131431
- help@gbclinics.co.uk
Clinic Hours:
Tuesday, Wednesday, Thursday & Friday : 10:00 AM – 8:00 PM || Saturday and Sunday: Booked appointments only
Say Goodbye to Shoulder Pain:
Inside GB Clinics’ Specialist Shoulder Clinic
Shoulder pain rarely arrives with fanfare. It doesn’t crash into your life like a broken bone or a sudden injury. More often, it arrives quietly. A slight stiffness when you brush your hair. A mild ache when reaching into the back seat. You think it’s nothing—maybe you slept oddly or lifted something wrong.
But then it’s still there the next day. And the one after that.
Gradually, it becomes part of how you move—hesitantly, guardedly. You avoid reaching overhead, you shift your sleeping position, you stop stretching in the mornings. And at some point, without meaning to, you start living around your shoulder pain instead of through it.
At GB Clinics, we see this often. And not because people aren’t paying attention—but because pain, when it comes slowly, is easy to underestimate.
We built our Specialist Shoulder Clinic for one reason: to offer clarity, comfort, and expert care to people who’ve been living with shoulder pain for too long. Not just symptom relief, but understanding. Because the shoulder, when examined properly, can often tell us a very clear story.
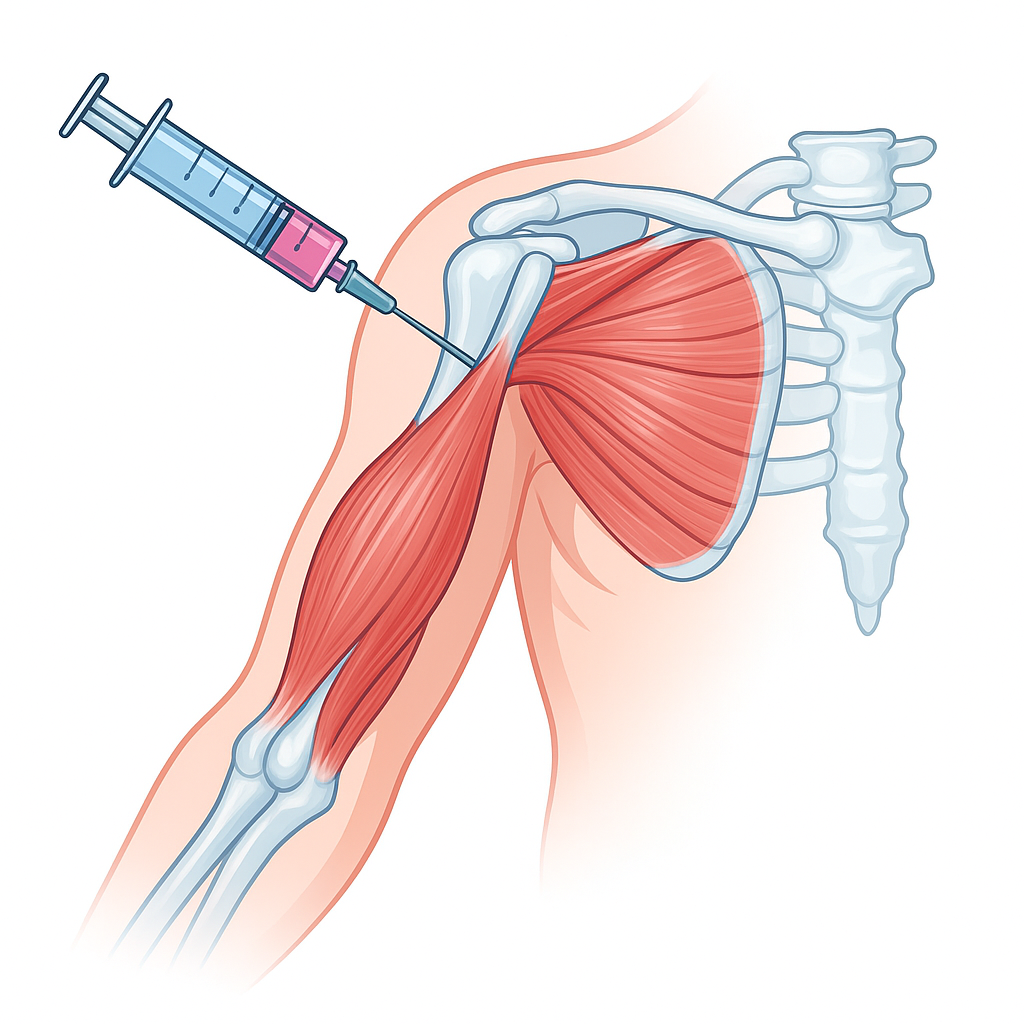
Understanding Shoulder Pain: Why It’s So Common
The shoulder is the most mobile joint in your body. It’s designed to lift, rotate, stretch, swing. But with that mobility comes complexity. The joint depends on a delicate balance of bones, ligaments, tendons, muscles, and fluid-filled sacs—all working in harmony.
When that balance is disrupted, even slightly, pain can follow.
At GB Clinics, some of the most common shoulder conditions we diagnose and treat include:
Frozen Shoulder (Adhesive Capsulitis)
This condition starts quietly—usually with stiffness or discomfort when reaching overhead. But over weeks or months, it progresses. Movements that once felt natural now feel restricted. The shoulder feels “stuck,” especially at night. Sleep becomes disrupted. Daily tasks, like dressing or lifting a bag, become frustrating.
Frozen shoulder occurs when the capsule surrounding the joint becomes inflamed and tightens. The result? Restricted movement and significant pain. It can last a long time without intervention. But with the right treatment and rehabilitation, recovery is very achievable—and often faster than people expect.

Rotator Cuff Tendinopathy and Tears
The rotator cuff is a group of four small muscles that stabilise and power your shoulder. They work every time you lift, carry, or reach. These tendons are prone to overuse, strain, and degeneration—especially with age or repetitive movement.
Injuries can range from mild inflammation to partial or full-thickness tears. People often describe it as a deep, dull ache made worse by lifting the arm, especially to the side or overhead. Weakness can follow. And without proper care, small injuries here can worsen over time.
Shoulder Osteoarthritis
Although we often associate arthritis with knees and hips, the shoulder isn’t immune. Over time, cartilage within the shoulder joint can wear down, leading to pain, stiffness, and reduced mobility.
This condition is often gradual and gets mislabelled as “just ageing.” But arthritis isn’t something to simply live with. There are effective treatments—many of which don’t involve surgery—that can greatly improve comfort and function.
Why We Always Start with Imaging
One of the most common things patients tell us is:
“I’ve had this pain for months. I’ve seen people. I’ve tried exercises. But no one’s told me exactly what’s wrong.”
That frustration is understandable. Because shoulder pain—without imaging—is hard to fully understand. Clinical tests help, but without visual confirmation, we’re working in the dark.
That’s why we use real-time musculoskeletal ultrasound at the very first visit.
This isn’t the kind of scan you have to wait weeks for. It’s done during your appointment, while you’re in the room. And unlike an MRI or X-ray, ultrasound is dynamic—we can watch your shoulder move, spot abnormalities, and understand how the tissues behave under real conditions.
- With ultrasound, we can:
- Identify tendon tears or fraying
- Detect fluid in the bursa (bursitis)
- See signs of calcification
- Spot joint impingement or thickening
- Visualise frozen capsule tightening
- It also allows us to guide injections with pinpoint precision, reducing pain and improving outcomes.
What Happens Next: A Care Pathway Designed Around You
Once we understand the cause of your shoulder pain, we work with you to build a plan. And if treatment is appropriate that same day—we get started.
Here’s how the process usually flows:
- Specialist Consultation:
You’re seen by a clinician with deep experience in shoulder diagnosis. We take the time to hear your story. When did the pain begin? What makes it worse? How is it affecting your day-to-day? We look, we listen, and we examine.
- Ultrasound Assessment:
We perform a dynamic scan while you move your shoulder. You can see the images in real time. We’ll explain what we’re seeing—no jargon, just clarity.
- Diagnosis and Planning:
We tell you exactly what’s going on. You’ll leave understanding not only the diagnosis, but also why it hurts, what your options are, and what steps come next.
- Treatment – Often Same Day:
Depending on the condition, we may offer treatment right away. That might include:
Ultrasound-Guided Steroid Injections – To reduce inflammation and pain in targeted areas like bursae, tendons, or the joint capsule.
Barbotage for Calcific Tendonitis – Using a fine needle to break up and flush out calcium deposits within a tendon. A minimally invasive procedure, often providing immediate relief.
Hydrodistension for Frozen Shoulder – A carefully delivered fluid injection to stretch the tight joint capsule and reduce stiffness.
PRP (Platelet-Rich Plasma) – A regenerative technique using your own blood’s healing cells, injected directly into damaged tissue.
- Rehabilitation Support:
No shoulder treatment is complete without movement. That’s why we work closely with our in-house physiotherapy team to tailor a rehabilitation plan that suits your pace, pain levels, and goals.
We don’t hand out one-size-fits-all sheets. We work with you. Because every shoulder is different, and so is every recovery.
Why Early Treatment Matters
Shoulder pain is often dismissed as something that will “settle on its own.” And sometimes, it does. But when pain lingers beyond a few weeks—or starts limiting your activity or sleep—it deserves proper attention.
The longer pain continues, the more it changes how you move. And when movement patterns change, secondary problems often follow: muscle weakness, neck tension, back strain. Early diagnosis helps break that cycle before it begins.
What Makes GB Clinics Different?
- We know there are other options out there. But here’s what patients tell us they value most:
- Consultant-led care from experienced MSK clinicians
- Real-time ultrasound during your visit
- Immediate diagnosis with a clear explanation
- Ultrasound-guided procedures for precision and safety
- Regenerative therapies like PRP available in-house
- A seamless path from consultation to rehab
- Free 2-hour parking and a calm, supportive environment
- A team that listens first, and treats second
- We don’t rush appointments. We don’t overpromise. We focus on doing what’s right, one shoulder at a time.
If You’re Living with Shoulder Pain…
Whether your pain started yesterday or a year ago, you don’t have to keep living around it. You don’t have to stretch your arm carefully, sleep in odd positions, or avoid doing things you used to enjoy.
You just need the right information. And the right care.
We’re here to provide both.

Book Your Appointment Today
Let’s take a proper look. Let’s understand what’s going on. And let’s begin the work of getting your shoulder—and your movement—back.
We’re ready when you are.